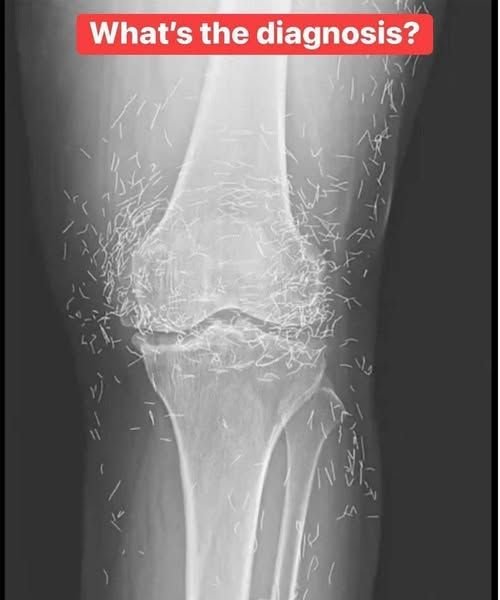
Chronic Knee Pain in a 65-Year-Old Woman After Months of No Relief: What the X-Ray Most Likely Shows
65-year-old woman with chronic knee pain and no relief from treatment—learn the most likely diagnosis, X-ray findings, and next steps for care.
When Knee Pain Stops Being “Just Aging”
Chronic knee pain in older adults is often dismissed too quickly.
“It’s just age.”
“Try some painkillers.”
“Maybe some alternative therapy will help.”
But when pain persists for months—even after multiple treatments including traditional approaches—it usually signals something more structural happening inside the joint.
In this case, a 65-year-old woman presents with long-standing knee pain that did not improve with traditional Chinese medicine or other conservative therapies. An X-ray was taken.
So what’s going on?
Let’s break it down like a clinician would—carefully, logically, and without jumping to conclusions.
The Most Likely Diagnosis: Knee Osteoarthritis
Based on the age group, symptom duration, and treatment resistance, the most likely diagnosis is:
osteoarthritis knee
This is by far the most common cause of chronic knee pain in adults over 60.
It is not an inflammatory disease in the autoimmune sense. Instead, it is a degenerative “wear-and-tear” condition where cartilage gradually breaks down over time.
Why Osteoarthritis Fits This Case So Well
Let’s connect the clinical clues:
1. Age Factor (65 years old)
Osteoarthritis risk increases significantly after age 50 due to cumulative joint stress.
2. Chronic Progression
Months of pain suggest a slow degenerative process, not an acute injury.
3. Poor Response to Treatment
Traditional therapies—including herbal or symptomatic treatments—may temporarily reduce discomfort but do not reverse cartilage loss.
4. Typical Joint Involvement
The knee is one of the most commonly affected joints due to weight-bearing stress.
What the X-Ray Typically Shows in Osteoarthritis
Although we don’t have the actual image here, classic knee osteoarthritis findings on X-ray include:
Key Radiological Features:
- Joint space narrowing (loss of cartilage cushion)
- Osteophytes (bone spurs along joint edges)
- Subchondral sclerosis (increased bone density under cartilage)
- Subchondral cysts (fluid-filled bone changes in advanced cases)
These findings develop gradually and correlate strongly with symptoms like stiffness, pain during movement, and reduced mobility.
Why the Pain Becomes Chronic
Osteoarthritis pain is not constant in the same way for everyone, but it tends to follow a pattern:
Early Stage:
- Mild stiffness in the morning
- Pain after long activity
Middle Stage:
- Pain during walking or climbing stairs
- Reduced knee flexibility
Advanced Stage:
- Pain even at rest
- Difficulty standing or bending
- Possible joint deformity
The key issue is that cartilage does not regenerate effectively once significantly damaged.
Why Traditional Treatments Often Fail Alone
In many regions, patients try multiple non-surgical approaches before getting a clear diagnosis.
These may include:
- Herbal medicine
- Massage therapy
- Topical treatments
- Pain relief gels
While these can help with symptom relief, they do not address the underlying mechanical issue: loss of cartilage and joint space narrowing.
That’s why pain often returns once treatment stops.
Other Possible Diagnoses (But Less Likely Here)
Even though osteoarthritis is the leading suspicion, clinicians always consider alternatives.
1. Rheumatoid Arthritis
An autoimmune condition that typically:
- Affects both knees symmetrically
- Causes morning stiffness lasting over an hour
- Shows inflammatory changes rather than wear-and-tear on X-ray
Less likely in this case due to age and presentation pattern.
2. Meniscal Degeneration or Tear
Common in older adults but usually:
- More localized pain
- May follow an injury
- Less likely to cause widespread chronic symptoms for months without fluctuation
3. Gout or Pseudogout
Typically presents as:
- Sudden flare-ups
- Severe redness and swelling
- Not a constant months-long pain pattern
What Actually Causes Knee Osteoarthritis?
Osteoarthritis is not just “old age.” It develops due to a combination of factors:
Mechanical Stress
Years of walking, standing, squatting, and lifting gradually wear down cartilage.
Biological Aging
Cartilage becomes less resilient and slower to repair.
Weight Load
Excess body weight increases pressure on knee joints significantly.
Previous Injuries
Old ligament or meniscus injuries increase future risk.
Genetics
Some individuals are predisposed to faster cartilage degeneration.
What Happens Inside the Joint Over Time
A healthy knee has smooth cartilage that allows bones to glide effortlessly.
In osteoarthritis:
- Cartilage starts thinning
- Bone surfaces become exposed
- Friction increases
- The body forms bone spurs (osteophytes)
- Inflammation develops in surrounding tissue
This cycle leads to pain and stiffness.
Step-by-Step Clinical Approach to This Patient
If this patient were evaluated in a modern clinic, the process would typically include:
Step 1: Physical Examination
- Joint tenderness
- Reduced range of motion
- Crepitus (grinding sensation)
Step 2: Imaging (X-ray)
Confirms structural changes like joint space narrowing.
Step 3: Pain Assessment
Understanding severity, triggers, and functional limitations.
Step 4: Treatment Planning
Based on severity stage.
Management Strategy: What Actually Helps
Treatment is not one-size-fits-all. It depends on severity.
1. Lifestyle and Weight Management
Even modest weight loss reduces knee load significantly.
2. Physical Therapy
Strengthening surrounding muscles—especially quadriceps—helps stabilize the joint.
3. Pain Management
Options may include:
- Topical anti-inflammatory gels
- Oral pain relievers when necessary
- Joint injections in some cases
4. Assistive Devices
Knee braces or walking support can reduce pressure during movement.
5. Advanced Options
In severe cases where mobility is significantly reduced:
- Joint injections
- Minimally invasive procedures
- Partial or total knee replacement surgery
Common Mistakes Patients Make
1. Ignoring Early Symptoms
Delaying treatment allows progression.
2. Over-Reliance on Passive Therapies
Massage or herbal remedies alone cannot reverse structural damage.
3. Avoiding Movement Completely
Complete rest weakens muscles and worsens stiffness.
4. Delaying Imaging
X-rays provide clarity and help guide proper treatment.
Real-World Scenario
A 68-year-old retired teacher experiences similar symptoms:
- Gradual knee pain over 1 year
- Difficulty climbing stairs
- Temporary relief from herbal oils
X-ray confirms moderate osteoarthritis.
With a combination of:
- Physiotherapy
- Weight reduction
- Strength training
Her pain reduces significantly within months, and she regains mobility.
Why Early Diagnosis Matters
Osteoarthritis cannot always be reversed—but progression can be slowed significantly.
Early detection helps:
- Preserve joint function
- Delay surgery
- Reduce long-term pain
- Improve quality of life
Future Outlook (2026 and Beyond)
Medical research is increasingly focused on:
- Cartilage regeneration therapies
- Stem cell-based joint repair
- Biologic injections to slow degeneration
- Improved non-surgical pain control methods
While not yet universal, these developments show promise for future treatment options.
Frequently Asked Questions
1. Is osteoarthritis reversible?
No, but symptoms and progression can be managed effectively.
2. Why does knee pain get worse with age?
Because cartilage naturally wears down and repair slows over time.
3. Can exercise make it worse?
Incorrect exercise can, but proper strengthening improves symptoms.
4. Is surgery always needed?
No, only in advanced or disabling cases.
5. What is the best treatment?
A combination of lifestyle changes, physiotherapy, and medical support.
6. Does weather affect knee pain?
Many patients report increased stiffness in cold or damp conditions.
7. Can supplements rebuild cartilage?
No strong evidence supports full cartilage regeneration from supplements alone.
8. How do X-rays confirm diagnosis?
They show structural changes like joint space narrowing and bone spurs.
Action Checklist
Do This:
- Strengthen leg muscles through guided exercise
- Maintain healthy body weight
- Stay physically active with low-impact movement
- Use proper knee support if needed
- Get imaging early if pain persists
Avoid This:
- Long-term inactivity
- Relying only on pain relief creams or herbal remedies
- Ignoring worsening symptoms
- Delaying medical evaluation
Conclusion: The X-Ray Isn’t Just an Image—It’s a Timeline
In a 65-year-old woman with chronic knee pain unresponsive to treatment, the most likely explanation is osteoarthritis—a gradual, mechanical breakdown of the joint over time.
The X-ray doesn’t just show damage.
It shows a story of years of stress, movement, and wear.
But it also shows something else:
A starting point for management.
Knee osteoarthritis isn’t the end of mobility—it’s a signal to shift from symptom relief to structured joint preservation.
If this reflects what you or someone you know is experiencing, early evaluation and targeted management can make a meaningful difference in long-term mobility and comfort.